Arthritis is one of the most misunderstood words in medicine. Most people use it as a catch-all term for joint pain, but not all arthritis is the same. Rheumatoid arthritis (RA) and osteoarthritis (OA) are two of the most common forms — and while they share some surface-level similarities, they are fundamentally different diseases with distinct causes, progressions, and treatments. Understanding the difference could change the way you approach your care.
Arthritis is one of the most misunderstood words in medicine. Most people use it as a catch-all term for joint pain, but not all arthritis is the same. Rheumatoid arthritis (RA) and osteoarthritis (OA) are two of the most common forms — and while they share some surface-level similarities, they are fundamentally different diseases with distinct causes, progressions, and treatments. Understanding the difference could change the way you approach your care.
What Is Osteoarthritis?
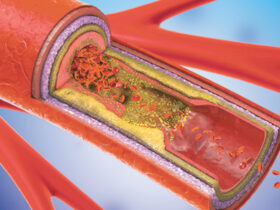
Osteoarthritis is the most prevalent form of arthritis, affecting over 32 million adults in the United States alone. It is a degenerative joint disease — meaning it develops as cartilage, the protective cushion between bones, gradually wears down over time. As that cushion erodes, bones begin to rub against each other, causing pain, stiffness, and reduced range of motion.
OA is primarily driven by mechanical wear and tear. Risk factors include age, excess body weight, previous joint injuries, and repetitive physical activity. It most commonly affects the knees, hips, hands, and spine. Symptoms tend to worsen with activity and improve with rest, and joint stiffness in the morning typically resolves within 30 minutes.
OA does not affect the whole body — it is a localized disease. There is no widespread inflammation, no immune system attack, and it does not damage organs beyond the joints.
What Is Rheumatoid Arthritis?
Rheumatoid arthritis is an entirely different condition. It is an autoimmune disease, meaning the body’s immune system mistakenly attacks the lining of its own joints — a tissue called the synovium. This triggers chronic inflammation that can destroy cartilage, erode bone, and cause permanent joint deformity if left untreated.
Unlike OA, RA is a systemic disease. It can affect the eyes, lungs, heart, and skin in addition to the joints. It typically presents symmetrically — if the right knee is affected, the left knee usually is too. Morning stiffness in RA often lasts longer than an hour, sometimes throughout the entire day. Fatigue, fever, and a general feeling of illness are also common.
RA can affect people at any age, including children (juvenile idiopathic arthritis), though it most commonly develops between the ages of 30 and 60. Women are two to three times more likely to be diagnosed than men.
Key Differences at a Glance
Osteoarthritis (OA):
• Degenerative joint disease caused by cartilage wear and tear
• Develops gradually, most often after age 50
• Morning stiffness typically resolves within 30 minutes
• Affects joints asymmetrically and locally
• Blood markers usually appear normal
• Rarely causes systemic (whole-body) effects
Rheumatoid Arthritis (RA):
• Autoimmune disease where the immune system attacks joint lining
• Can develop at any age, most commonly between 30–60
• Morning stiffness lasts over an hour, sometimes all day
• Affects joints symmetrically (both sides of the body)
• Elevated blood markers: RF, anti-CCP, and CRP
• Frequently causes systemic effects including fatigue, fever, and organ involvement
Why the Distinction Matters
Misidentifying one condition as the other can lead to delayed or ineffective treatment. OA is managed primarily through lifestyle changes, physical therapy, pain relief, and in advanced cases, joint replacement surgery. RA, on the other hand, requires disease-modifying antirheumatic drugs (DMARDs) and often biologic therapies to halt immune system damage — treatments that are completely unnecessary and inappropriate for OA.
Early, accurate diagnosis is critical for RA in particular. Joint damage from RA can begin within the first year of disease onset, and early intervention dramatically improves long-term outcomes.
When to Seek Help
If you are experiencing persistent joint pain, swelling, or stiffness — especially if it is symmetric, accompanied by fatigue, or accompanied by morning stiffness
Key Differences at a Glance
Osteoarthritis (OA):
• Degenerative joint disease caused by cartilage wear and tear
• Develops gradually, most often after age 50
• Morning stiffness typically resolves within 30 minutes
• Affects joints asymmetrically and locally
• Blood markers usually appear normal
• Rarely causes systemic (whole-body) effects
Rheumatoid Arthritis (RA):
• Autoimmune disease where the immune system attacks joint lining
• Can develop at any age, most commonly between 30–60
• Morning stiffness lasts over an hour, sometimes all day
• Affects joints symmetrically (both sides of the body)
• Elevated blood markers: RF, anti-CCP, and CRP
• Frequently causes systemic effects including fatigue, fever, and organ involvement
Why the Distinction Matters
Misidentifying one condition as the other can lead to delayed or ineffective treatment. OA is managed primarily through lifestyle changes, physical therapy, pain relief, and in advanced cases, joint replacement surgery. RA, on the other hand, requires disease-modifying antirheumatic drugs (DMARDs) and often biologic therapies to halt immune system damage — treatments that are completely unnecessary and inappropriate for OA.
Early, accurate diagnosis is critical for RA in particular. Joint damage from RA can begin within the first year of disease onset, and early intervention dramatically improves long-term outcomes.
When to Seek Help
If you are experiencing persistent joint pain, swelling, or stiffness — especially if it is symmetric, accompanied by fatigue, or accompanied by morning stiffness lasting more than 30 minutes — do not assume it is simply “wear and tear.” A rheumatologist can perform blood tests, imaging, and a clinical evaluation to determine exactly what type of arthritis you have and create a personalized treatment plan.
At RheumCare™, our specialists are dedicated to helping patients navigate complex rheumatic conditions with precision, compassion, and the latest evidence-based care. Because knowing what you have is the first step to feeling better.
Dr. Alain Alvarez
Bilingual in English and Spanish, Dr. Alvarez was born in Havana, Cuba and was raised in Miami, Florida. Dr. Alvarez graduated Phi Kappa Phi with a Bachelor of Science Degree in Microbiology and Immunology, and a medical degree from the University of Miami. He completed his residency in internal medicine at the Mayo Clinic in Jacksonville, Florida and completed his rheumatology fellowship training at the University of Minnesota.
An avid sports fan, especially college football, Dr. Alvarez has a keen interest in providing non-surgical orthopedic alternatives to his patients. He also holds a special interest in musculoskeletal ultrasound for which he has undergone additional training to be certified both nationally and internationally in the application of this technology for the treatment of rheumatic diseases. His practice consists of general adult rheumatology with a focus on inflammatory arthritis such as rheumatoid arthritis, psoriatic arthritis, lupus, polymyalgia rheumatica, ankylosing spondylitis, and vasculitis. He is also a willing participant and sub-investigator for numerous clinical trials.
Dr. Alvarez is a member of the Florida Society of Rheumatology, American Institute of Ultrasound in Medicine, American College of Rheumatology, Collier County Medical Society and Florida Medical Association.
Now accepting new patients
6605 Hillway Circle,
Unit 101 Naples, FL 34112
239-262-6550
www.rheumcare.net