By Dr. Ron Adduru, DPM – Family Foot & Leg Center
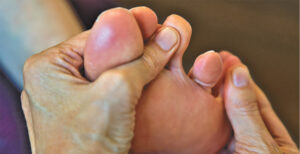 If you’ve spent years “walking on eggshells”—or rather, walking on the outside of your foot to avoid bending your big toe—you aren’t alone.
If you’ve spent years “walking on eggshells”—or rather, walking on the outside of your foot to avoid bending your big toe—you aren’t alone.
In my Sarasota practice, hallux rigidus (big toe arthritis) is a common, frustrating condition I treat. It’s the medical term for a stiff big toe caused by degenerative arthritis. When the smooth cartilage in that joint wears thin, bone rubs against bone, creating painful spurs (osteophytes) and stripping away your ability to walk, run, or wear your favorite shoes.
For decades, the surgical options were limited to a choice between two extremes: lose your motion or take a gamble on a “miracle” plastic plug. Today, I am proud to offer a groundbreaking alternative at Family Foot & Leg Center:
Hallux Rigidus Arthroplasty with Interpositional Dermal Allograft
This procedure resects prominent arthritic bone and releases contracted soft tissues within the 1st metatarsophalangeal joint to increase range of motion. A Dermal Allograft is then applied and secured to the 1st metatarsal head with knotless suture anchors, creating a protective covering and cushioning within the joint and metatarsal-sesamoid articulation.
Postoperatively, the patient can immediately bear weight and ambulate in a surgical shoe. The skin is closed with absorbable sutures, with healing taking approximately 2-3 weeks. While stiffness and swelling are normal, physical therapy accelerates recovery, improving range of motion and function with minimal downtime.
The “Gold Standard” That Isn’t Always Golden:
Joint Fusion
Historically, the most reliable treatment for end-stage hallux rigidus was arthrodesis, or joint fusion. By removing remaining cartilage and using plates and screws to lock the bones, we eliminate painful rubbing.
While fusion provides excellent pain relief, it comes at a significant cost: total loss of motion. For a high-level athlete, a yoga enthusiast, or someone wanting to wear a slight heel at St. Armands Circle, a fused toe can feel like a mechanical failure. You lose “push-off” power, and stress often migrates to the smaller toe joints or ankle, leading to secondary issues.
The Failed Promise of Synthetic Cartilage
In the last decade, many patients were sold on the idea of Synthetic Cartilage Implants (like the Cartiva hydrogel plug). It was marketed as a “game-changer”—a simple 20-minute procedure to replace cartilage with a synthetic spacer.
Unfortunately, the real-world data has told a different story. In my clinical experience and according to recent medical literature, these implants have seen alarmingly high failure rates. The synthetic material often:
• Subsides: It sinks into the bone like a pebble in wet sand.
• Fragments: It breaks apart, causing a massive inflammatory reaction.
• Fails to relieve pain: Many patients end up back in the operating room within two years to have the implant removed and the joint fused anyway — often with more bone loss than they started with.
The Breakthrough: Dermal Allograft Interposition
We needed a solution that preserved motion without the risks of synthetic “foreign bodies.” That solution is the Dermal Allograft.
Instead of a plastic plug or a metal hinge, we use a specialized, acellular human dermal matrix—essentially a biological “cushion” derived from donated human tissue. This graft acts as a biological spacer that resurfaces the joint.
How the Procedure Works
During the procedure, I perform a thorough cheilectomy to remove the painful bone spurs and “clean out” the joint. I then carefully wrap the metatarsal head (the ball of the foot) with the dermal allograft.
Think of it like adding a high-tech, biological gasket to a worn-out hinge. Because this is human tissue, your body doesn’t fight it like a synthetic implant. Instead, it provides a smooth, durable gliding surface.
Why This is the Future of Foot Surgery
The advantages of this technique over old methods are clear:
1. Motion Preservation: Unlike fusion, you keep the ability to bend your toe naturally.
2. No “Foreign Body” Rejection: Since it is a biological graft, we avoid the fragmentation and bone erosion seen with synthetic implants.
3. Joint Sparing: If the arthritis were ever to progress decades later, we haven’t burned any bridges. We haven’t removed large chunks of bone, making future options much simpler.
4. Faster Recovery: Many of my patients are back in a supportive sneaker much sooner than those undergoing a traditional fusion.
Your Next Step Toward Pain-Free Movement
You don’t have to choose between chronic pain or a “dead” toe. If you’ve been told fusion is your only option, let’s discuss if a dermal allograft is right for you.
Would you like me to help you schedule a consultation at our Sarasota office to evaluate your big toe pain and discuss your surgical options?
Disclaimer: This content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health care provider with any questions you may have regarding a medical condition.
Dr. Ron Adduru is a podiatrist at Family Foot & Leg Center in Sarasota, Florida, specializing in complex wound care and deformity reconstruction. He is committed to helping the Sarasota community remain active and healthy.
3110 Fruitville Commons Blvd
Suite 102
Sarasota, FL 34240
(239) 430 – 3668 (FOOT)
www.NaplesPodiatrist.com