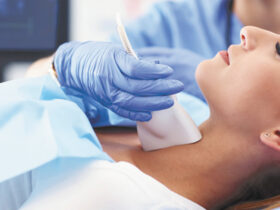
Beware of falling into trap of thinking there’s a ‘stereotypical high-risk patient’
Anyone can suffer a stroke. Literally anyone.
Stroke is not confined to a specific age group or a stereotypical “high-risk” patient. While there is a tendency to associate stroke with older adults or individuals with obvious health issues, that framing is incomplete—and a bit misleading.
“Yes, there are well-established risk factors like hypertension, diabetes and smoking, but stroke can also occur in individuals who don’t fit that profile at all,” says Megan Walsh, DPT, NCS, a Clinical Assistant Professor in Florida Gulf Coast University’s Marieb College of Health and Human Services who is recognized as a Board Certified Neurologic Clinical Specialist by the American Board of Physical Therapy.
“Younger, otherwise healthy people can experience strokes due to less obvious mechanisms like embolic events, cardiac rhythm disturbances, vascular abnormalities or even spontaneous arterial injury. In some cases, there isn’t a clear, immediately identifiable cause. What complicates this further is that stroke doesn’t always present in the dramatic way people expect. It’s not always a sudden collapse or complete paralysis. It can be subtle, such as sudden dizziness, difficulty with balance, changes in vision or mild speech disturbances.”
Those presentations are easy to dismiss, especially when the person doesn’t “look like” someone at risk. So the idea that “anyone can suffer a stroke” is less about creating alarm and more about correcting that bias.
“It’s a reminder that stroke is fundamentally a neurological emergency defined by its presentation, not by the person it happens to,” says Walsh, who is certified in Neurodevelopmental Treatment (NDT) by the Neurodevelopmental Treatment Association (NDTA). “If symptoms appear suddenly and don’t make sense, they deserve to be taken seriously, regardless of age or perceived health status.”
Walsh speaks from painful experience. She did not realize that babies could have a stroke—until her second daughter, Piper, was born full-term in 2009. Within 24 hours, doctors discovered that she was experiencing seizures that necessitated admission to the neonatal intensive care unit (NICU). A battery of tests determined that she had suffered a large stroke affecting the left side of her brain in an area known to control right-sided movement and speech.
Walsh begged the neurologist in the NICU to tell her and her husband that Piper would still be OK and be able to live a normal life. Of course, he could not do that, instead saying, “She will be anything from profoundly disabled to relatively normal. Time, early intervention and neuroplasticity will dictate her outcome.”
Piper made a phenomenal recovery. Now in 10th grade, she has participated in Irish dance, played club-level soccer and graced her school’s Honor Roll on several occasions.
Even before Piper’s ordeal, Walsh had developed a passion for helping people through difficult and often unforeseen circumstances. She became interested in stroke rehabilitation while working at the Rehab Hospital of the Pacific in Honolulu from 2005 to 2008. But it was not until Piper was born that she expanded that passion to include awareness and research.
From a healthcare provider and professor’s perspective, she believes stroke prevention is one of the areas where they can have the most meaningful impact in the community, because so many of the major risk factors are actually modifiable.
“Hypertension is still the leading contributor, so consistent blood pressure management—through medication when needed, but also through movement and lifestyle—is fundamental,” she says. “What we see clinically, though, is that these risks rarely exist in isolation. Physical inactivity, impaired glucose control and high cholesterol tend to cluster, creating a cumulative strain on the vascular system over time. Tobacco use and excessive alcohol intake further accelerate that process.
“What I consistently emphasize, both in the classroom and in practice, is that movement is not just a general wellness recommendation, but it is a targeted, evidence-based intervention. Regular aerobic activity and strength training directly improve blood pressure, insulin sensitivity and lipid profiles, which are all central to reducing stroke risk.
“There is also increasing recognition of the role that sleep quality and chronic stress play, particularly in conditions like obstructive sleep apnea, which often go under-identified. Ultimately, stroke prevention is not about a single behavior change. It is the cumulative effect of managing cardiovascular health over
time. The encouraging part is that even small, consistent changes in these modifiable factors can meaningfully reduce long-term risk.”
She says that when we talk about who is more susceptible to stroke, it’s important to frame it less as a specific “type” of person and more in terms of non-modifiable risk factors layered on top of an individual’s overall risk profile. Age remains the most significant non-modifiable factor, with risk increasing over time, but it’s critical to recognize that stroke is not exclusive to older adults.
“We are continuing to see strokes in younger populations, often because modifiable risks are present but under-recognized,” she says. “There are also important sex-based considerations. Women, for example, have unique risk periods related to pregnancy and the postpartum state, as well as considerations with hormonal contraception and migraine with aura, all of which can influence stroke risk through vascular and clotting mechanisms.
“In addition, race and ethnicity play a role, as African American adults in the United States experience higher stroke incidence and often at younger ages, which reflects both biological predispositions and broader social and healthcare access factors. Genetics and family history are also key non-modifiable contributors, particularly in individuals with inherited clotting disorders or early cardiovascular disease in first-degree relatives. These factors can increase baseline risk even in individuals who appear otherwise healthy.
“That said, these non-modifiable risks don’t act in isolation. They interact with modifiable factors like hypertension, physical inactivity, diabetes, dyslipidemia and tobacco use, which ultimately drive the majority of stroke risk. So while we can’t change age, sex, race or genetics, understanding how they influence baseline risk allows us to be more proactive and aggressive in managing the factors we can modify.”
FGCU
Marieb College of Health and Human Services
10501 FGCU Boulevard South, Fort Myers, FL 33965
(239) 590-1000 | fgcu.edu