Michael J. Petrocelli, D.P.M., F.A.C.F.A.S., C.W.S.P.
Board Certified Ankle and Foot Surgeon and Board Certified Wound Care Specialist
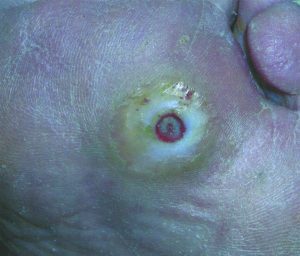 Millions of folks that have diabetes will suffer from diabetic foot ulcers more than once in their lifetimes. Diabetes is a progressive disease that is often not taken seriously enough; this is due in part to its increasingly growing diagnosis and commonality. This disease’s increase is particularly the case here in the United States where nearly 30 million people have the syndrome.
Millions of folks that have diabetes will suffer from diabetic foot ulcers more than once in their lifetimes. Diabetes is a progressive disease that is often not taken seriously enough; this is due in part to its increasingly growing diagnosis and commonality. This disease’s increase is particularly the case here in the United States where nearly 30 million people have the syndrome.
High blood sugar damages various organs within the body, but also has a severely adverse effect on nerves. This nerve damage happens when the blood supply is limited. The small blood vessels, which supply blood and nutrients to the nerves becomes impaired. When the nerves are no longer fed nutrients, they either die, or their signals to the brain are ineffective.
The lack of brain signaling from the nerve endings makes it difficult for a person to feel pain in their foot, so often injuries and these disorders are overlooked. This syndrome is called peripheral diabetic neuropathy.
Because of this nerve damage, people with diabetes are at a higher risk of developing foot ulcers. A foot wound may not sound overly alarming to most people, but foot ulcers can be life threatening. These small ulcers go undetected due to the lack of feeling. If a patient delays treatment, foot ulcers can lead to amputation, strokes, heart attacks and severe infections that can spread throughout the entire body.
How do the ulcers form?
Because of the nerve damage, the feet will most likely not secrete oils or sweat properly and can develop cracks and deep slits from dry skin. Calluses can also split, and once these issues start to take place, bleeding, infections and non-healing wounds develop on the bottom of the foot and toes. The lack of blood supply and the nerve issues, do not allow the wound to heal properly on its own. Along with this disorder, the individual will continue to put pressure on the foot; this rubbing action is similar to wearing a hole in your sock or shoe.
Symptoms of diabetic ulcers are often ambiguous because of the loss of feeling, but most often they include the following sensations in the foot or legs:
• Burning
• Numbness
• Sensations of cold/hot
• Stumbling
• Tingling
If foot ulcers are left untreated in diabetic patients, they can develop into gangrene. Unfortunately, in these cases, it is not uncommon for patients to need amputation of their toes, foot, or leg due to progressive infection. It is always best to see a podiatrist proactively if you have diabetes.
And if you are experiencing any foot sores, cuts or excessive cracks, you should schedule and appointment with your physician immediately.
Along with keeping your glucose levels regulated, the typical treatment options are:
• Antibiotics
• Grafts
• Hyperbaric oxygen treatments
• Saline debridement
• Surgery
• Therapeutic footwear
• Wound care
People with diabetes are encouraged to do self-checks on their feet daily. As soon as you notice any redness or wounds, it is imperative to see your podiatrist.
Collier Podiatry
Dr. Michael Petrocelli has been practicing podiatric medicine for well over 20 years. He is an expert in his field and a leader to his peers. If you are experiencing any foot pain or foot conditions, please contact Collier Podiatry.
Their kind and well-trained staff are ready to answer your questions and concerns and get you back on your feet again.
Collier Podiatry is available to answer your questions and make your appointment. Please visit their website at www.collierpodiatry.com, or call them at (239) 775-0019